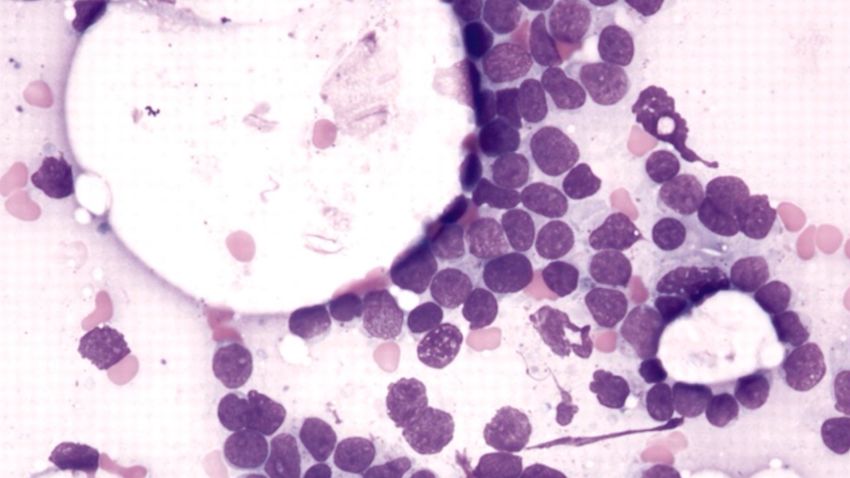
Story highlights
Kymriah works by genetically modifying a patient's own cells so they can attack the cancer
An advisory committee recommended the drug for approval in July
The US Food and Drug Administration approved a new leukemia treatment, which the agency considers the first gene therapy it has cleared to hit the market in the United States.
The treatment, called Kymriah, aims to give some patients a second chance after first-line drugs have failed. This may happen in up to a fifth of patients, according to the FDA.
Each dose of Kymriah contains a patient’s own immune cells, which are sent to a lab to be genetically modified using a virus. This therapy – known as chimeric antigen receptor T-cell therapy, or CAR-T – gives the cells the ability to recognize and kill the source of the cancer.
“We’re entering a new frontier in medical innovation with the ability to reprogram a patient’s own cells to attack a deadly cancer,” FDA Commissioner Dr. Scott Gottlieb said in a statement.
“We’ve never seen anything like this before and I believe this therapy may become the new standard of care for this patient population,” said Dr. Stephan Grupp, director of cancer immunotherapy at Children’s Hospital of Philadelphia, which spearheaded this research.
An FDA advisory committee had recommended the therapy for approval in July to treat the relapse of a blood cancer known as B-cell acute lymphoblastic leukemia, or ALL.
Based on available data, patients on the treatment have had an 89% chance of surviving at least six months and a 79% chance of surviving at least a year, with most being relapse-free at that point.
Almost 5,000 people were diagnosed with ALL in 2014, according to the US Centers for Disease Control and Prevention. More than half were children and teens. ALL is the most common type of cancer among children, according to the National Cancer Institute.
Most patients with ALL recover through other treatments such as radiation, chemotherapy and stem cells. But if the cancer recurs, the prognosis is poor.
“There has been an urgent need for novel treatment options that improve outcomes for patients with relapsed or refractory B-cell precursor ALL,” Novartis, the drug company that makes Kymriah, said in a statement.
“Kymriah is a first-of-its-kind treatment approach that fills an important unmet need for children and young adults with this serious disease,” Dr. Peter Marks, director of the FDA’s Center for Biologics Evaluation and Research, said in a statement.
The one-time treatment has a boxed warning for cytokine release syndrome or CRS, a life-threatening side effect that can cause blood pressure to drop dangerously low. It is caused by overactive genetically modified immune cells. The FDA said hospitals and clinics must become certified to distribute the treatment, meaning they are prepared to recognize and treat CRS and other potentially fatal neurological events. Novartis said it hopes to have an initial network of 20 treatment centers within a month with plans to expand that to 32 by the end of the year.
Kymriah has a $475,000 price tag; however, patients who do not respond within a month of treatment will not be charged, according to Novartis.
“Novartis is collaborating with (Centers for Medicaid Services) to make an outcomes-based approach available to allow for payment only when pediatric and young adult ALL patients respond to Kymriah by the end of the first month. Future potential indications would be reviewed for the most relevant outcomes-based approach,” the drug company said in a statement.
Join the conversation
On Wednesday, the FDA also expanded approval for another drug, tocilizumab, to treat CRS in patients 2 and older.
In the main study that informed the advisory committee’s decision in July, roughly half of 68 patients experienced high-grade CRS, though none died from it. Slightly fewer patients experienced neurological events, such as seizures and hallucinations.
Novartis is required to conduct followup study to assess the safety of the treatment long-term.